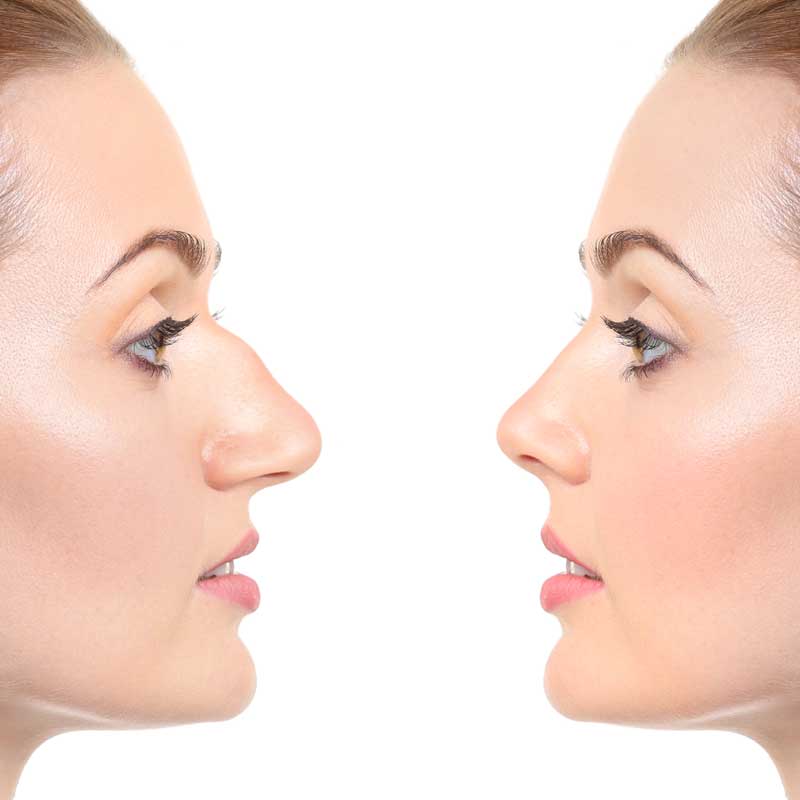
Rhinoseptoplasty is a surgical process designed to alter the shape and size of your nose, as well as narrow flared nostrils. Usually performed under general anesthesia.
Before surgery, it is essential that any blood-thinning medications be discontinued and an arrangement made for someone to drive you home after your operation.
Aesthetics
Rhinoplasty is one of the most frequently performed aesthetic surgeries to enhance facial appearance. It aims to alter the proportions of the nose so it fits better within its environment, keeping in balance with other facial features like eyes, ears and lips.
At the beginning of surgery, your surgeon will make an incision under each nostril in order to gain access to bone and cartilage structures that need changing. They then use special tools to alter those bones or cartilage structures as needed in order to alter its size or shape accordingly.
Techniques for increasing nasal tip projection may include shortening the length of lateral and medial crura by cartilage overlapping or placing a columellar strut (placing a rectangular piece of septal cartilage between them), while for decreasing bridge height there exist techniques like reducing dorsal hump height, reshaping your nose, or decreasing turbinates (spongy bones lining nasal passages) to increase airflow – creating a balanced yet natural-looking nose that complements your facial features.
Functionality
Crooked cartilage lines known as septums may lead to breathing issues for some individuals, especially snorers at night. Cosmetic modifications must not interfere with airflow through their nose; cosmetic rhinoplasty combined with septoplasty procedures such as Rhinoseptoplasty may help improve breathing in such instances.
Rhinoseptoplasty can correct crooked septa and reshape the nose for easier breathing, however its nasal structures can sometimes be fragile in thin patients, necessitating additional support such as grafts.
Before performing rhinoseptoplasty, a physician will conduct an assessment to ensure it is the appropriate solution. They will examine frontal, profile and basal views of the nose in detail to understand what achievable goals may be; discuss goals further with patient and use 3-D simulation software to demonstrate expected results – an important tool that helps patients understand what can be accomplished through rhinoseptoplasty while managing expectations accordingly.
Safety
Rhinoplasty is one of the more complex surgical procedures available. Complications may result in 5% to 15% of cases; most often due to instability of the septum.
Postoperative bleeding may be manageable with head elevation, nasal decongestants and compression techniques; severe bleeding that does not respond to these methods may require anterior tamponage and further analysis of the nasal dorsum.
Septal perforations is a serious threat that can range from minor discomfort, like whistling when breathing, to epistaxis or rhinitis due to disruptions of airflow through the nose. Preventing septal perforations requires meticulous manipulation of mucoperichondrial flaps during surgery procedures.
Rhinoplasty surgery should be carried out under general or local anesthesia and at an age when nasal structures have matured and won’t change significantly further. Prior to any rhinoplasty procedure being performed, preoperative photos must be taken for analysis, planning and medico-legal purposes; including frontal view photos as well as profiles and basal views for future reference.
Recovery
After having rhinoplasty surgery, it’s not unusual to experience some initial swelling in your nose and face due to how surgery impacts blood vessels and tissues; fortunately, however, this swelling typically subsides within one week of completion of your procedure.
At this stage, it is wise to avoid activities that could result in a blow to the nose, including contact sports and any physical activities where an accident could cause something to strike at it and hit you square in the nose, potentially inflicting injury as well as shifting internal packing stents or shifting their placement.
Your surgeon may use nasal packing, splints or an external cast to support your nose while it heals from surgery. They’ll usually remove them about seven days postoperatively when most major bruising has faded and your nose appears closer to its natural shape – so you can resume normal life afterwards.
Disclaimer: The content on this blog is intended for general informational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult qualified healthcare providers for personalized advice. Information regarding plastic surgery, dental treatment, hair transplant, and other medical procedures is educational and not a guarantee of results. We do not assume liability for actions taken based on blog content. Medical knowledge evolves; verify information and consult professionals. External links do not imply endorsement. By using this blog, you agree to these terms.